Chronic Fatigue Explained: Why You Feel Tired Even After Sleeping 8 Hours (and How to Fix It)

Chronic fatigue explained: find out why you feel exhausted after 8 hours of sleep, what causes it, and proven remedies to restore your energy levels for good.
Still Exhausted After a Full Night’s Sleep?

You slept a full 8 hours. You did everything right. You turned off your phone, went to bed at a decent time, and even skipped that late-night snack. And yet the alarm goes off and you feel like you barely slept at all. If this sounds familiar, you are not alone, and more importantly, you are not imagining it.
Chronic fatigue after sleeping is one of the most common, most frustrating, and most misunderstood health problems of our time. It shows up quietly, builds slowly, and tends to get brushed off as “just stress” or “part of getting older.” But waking up exhausted after a full night of sleep is your body sending a clear signal that something deeper is going on.
RECOMMENDED POST: How Exercise Improves Your Sleep Quality
In this article, we are going to break down exactly why that happens. We will look at the real causes of unrefreshing sleep and persistent tiredness, walk through the symptoms that tell you this is more than ordinary fatigue, and give you a practical, evidence-based plan to start reclaiming your energy. By the end, you will have real answers and real steps forward.
45% Of Americans report significant fatigue multiple times per week
1 in 50 People globally are estimated to have ME/CFS (Chronic Fatigue Syndrome)
91% Of ME/CFS cases in the US are estimated to go undiagnosed (CDC)
The Real Causes of Chronic Fatigue: Why You Feel Tired Even After Sleeping 8 Hours
Here is the single most important thing to understand about this problem: sleeping 8 hours and sleeping well are two completely different things. You can lie in bed for 8 or even 10 hours and still only get 3 or 4 hours of truly restorative sleep. That difference is where chronic fatigue begins for most people.
Undiagnosed Sleep Disorders
Sleep apnea is far more widespread than most people realize. The American Sleep Apnea Association estimates that 30 million Americans have it, with the majority undiagnosed. With sleep apnea, your airway partially or fully collapses during sleep, causing brief pauses in breathing. Your brain jolts itself awake to restore the airway, sometimes hundreds of times a night, without any memory of it in the morning. The result is that you spend 8 hours in bed and wake up feeling like you ran a marathon.
Restless Leg Syndrome, teeth grinding (bruxism), and periodic limb movement disorder can produce the same fragmented, non-restorative sleep pattern. These are all medical conditions with real treatments. They are not character flaws or signs of weakness.
Hormonal Imbalances Driving Persistent Tiredness
Your hormones are the invisible conductors of your energy levels throughout the day. An underactive thyroid gland, a condition called hypothyroidism, is one of the most frequent hormonal causes of constant tiredness. It is especially common in women. Low testosterone in men, adrenal hormone irregularities, and the estrogen and progesterone fluctuations of perimenopause can all produce fatigue that no amount of sleep seems to touch.
UK / Canada / Australia note: In the UK, thyroid testing (TSH and free T4) is ordered routinely through NHS GPs. In Canada, thyroid panels are covered by provincial health plans such as OHIP in Ontario. In Australia, thyroid function tests are Medicare-rebatable with a GP referral. Ask for a full thyroid panel, not just TSH, if you suspect a thyroid issue.
Nutritional Deficiencies and Their Hidden Impact
Iron deficiency is the world’s most common nutritional deficiency according to the World Health Organization. Even when levels are low-normal (technically not anemic), reduced iron can impair oxygen delivery to cells, cause brain fog, and leave you feeling heavy and slow. It is particularly common in people who menstruate, vegetarians, vegans, and anyone with conditions like Celiac disease that impair nutrient absorption.
Vitamin B12 deficiency is another major driver of unexplained tiredness. B12 is essential for nerve function and red blood cell production. Low B12 often presents as fatigue, mental fog, mood changes, and tingling sensations in the limbs. Vitamin D deficiency is also strongly associated with fatigue, particularly in people living in northern latitudes where sun exposure is limited for months at a time.
Chronic Stress and a Nervous System That Cannot Switch Off
When you are under sustained psychological stress, your sympathetic nervous system stays in a low-level “alert” state. This is called hyperarousal. It means that even when you fall asleep, your brain never fully descends into the deep restorative stages it needs. People managing chronic work pressure, anxiety, caregiving demands, or unresolved trauma commonly experience this exact pattern.
The cruel irony is that fatigue makes stress harder to manage, and ongoing stress keeps making the fatigue worse. Breaking that cycle requires a deliberate, multi-pronged approach, which we will cover fully in the remedies section.
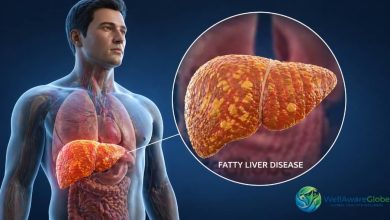
Underlying Medical Conditions That Cause Constant Tiredness
Persistent fatigue is also a documented symptom of type 2 diabetes, heart disease, chronic kidney disease, autoimmune conditions like lupus and rheumatoid arthritis, fibromyalgia, and Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS). ME/CFS is a serious, complex illness formally recognized by the CDC and the World Health Organization. It affects millions of people globally and is not, in any way, simply a matter of needing more willpower or a better attitude.
RECOMMENDED POST: Type 2 Diabetes: 7 Early Warning Signs, Causes, and Proven Natural Ways to Control Blood Sugar
Symptoms of Chronic Fatigue: How to Know It Is More Than Ordinary Tiredness
Everyone gets tired. After a long week, a travel-heavy schedule, or a season of stress, low energy is expected. But chronic fatigue has a different quality to it. It persists, it is resistant to rest, and it tends to touch multiple areas of your life at once.
Here are the most important signs that what you are experiencing goes beyond normal tiredness:
Waking up unrefreshed:
You sleep a full night and feel no better in the morning than when you went to bed.
Brain fog:
Difficulty concentrating, slow thinking, poor memory, and mental heaviness
Post-exertional malaise:
Feeling significantly worse after even mild physical or mental activity
Muscle and joint aches:
Unexplained body heaviness or aching not tied to exercise or injury
Mood disturbances:
Increased irritability, low mood, or emotional flatness alongside physical fatigue
Frequent headaches:
Recurring headaches or a persistent heavy feeling around the eyes or temples
Duration is one of the most important factors here. Most medical guidelines use a 6-month threshold as a general benchmark: if you have experienced persistent unexplained fatigue for 6 months or more, a full medical evaluation is warranted. That said, you should seek care sooner if symptoms are severe, rapidly worsening, or accompanied by warning signs like unexplained weight loss, chest pain, or night sweats.
How to Fix Chronic Fatigue and Stop Feeling Tired Even After Sleeping 8 Hours
This is the section most people come for, and we are not going to give you vague advice about “practicing good sleep hygiene.” These are targeted strategies, each with a specific mechanism and real evidence behind them. They are organized from the most foundational to the more advanced.
Step 1: Honestly Assess Your Sleep Quality
The first step is getting real data. Keeping a sleep diary for two weeks, noting your bedtime, wake time, how rested you feel each morning on a scale of 1 to 10, and any notable disruptions, often reveals patterns that are not obvious in the moment. Many people are surprised to find that what they thought was 8 hours of sleep is consistently 6.5 hours of actual time asleep once they account for lying awake, waking in the night, and early morning waking.
Consumer sleep trackers from brands like Fitbit, Garmin, and the Oura Ring can give a useful (if imperfect) window into your sleep stages. If you suspect sleep apnea based on symptoms like snoring, waking with headaches, or a partner noticing pauses in your breathing, ask your doctor about a sleep study. Many regions now offer at-home sleep testing as an accessible first step.
UK / Canada / Australia note: In the UK, home sleep studies can be arranged through NHS Sleep Clinics or private referral. In Canada, home sleep apnea testing is increasingly covered by provincial health plans. In Australia, many polysomnography tests are Medicare-rebatable with a GP referral.
Step 2: Build Better Sleep Architecture
Improving how your brain moves through sleep stages does not require medication. The following habits have the strongest research backing for improving sleep quality specifically:
Anchor your wake time. Choose a fixed wake time, including weekends, and stick to it. A consistent wake time is the most powerful regulator of your circadian rhythm, more effective than trying to manage a consistent bedtime. Everything else follows from this one habit.
Get morning sunlight within 60 minutes of waking. Natural light exposure in the morning suppresses residual melatonin and sets your internal clock for the day. Even 10 minutes outside on a cloudy morning is measurably effective.
Lower your bedroom temperature. Core body temperature must drop by roughly 1 to 2 degrees Fahrenheit (about 0.5 to 1 degree Celsius) for deep sleep to begin. Aim for a room temperature between 60 and 68 degrees Fahrenheit (15 to 20 degrees Celsius).
Cut off caffeine after 12 noon. Caffeine has a half-life of approximately 5 to 6 hours. That afternoon coffee you used to power through the 3 PM slump is still partially active in your bloodstream at 9 PM and is fragmenting your deep sleep.
Treat insomnia with CBT-I before medication. Cognitive Behavioral Therapy for Insomnia (CBT-I) is recognized by the American College of Physicians as the first-line treatment for chronic insomnia. It outperforms sleep medications in long-term outcomes and has no side effects. Free and low-cost CBT-I programs are available online and through apps like Sleepio.
Step 3: Get a Targeted Blood Panel
Before spending money on any supplements, invest in knowledge first. A basic blood panel for fatigue investigation should include: a complete blood count (CBC), ferritin (the storage form of iron, more informative than basic iron), serum vitamin B12, 25-hydroxyvitamin D, thyroid function (TSH and free T4), and a fasting blood glucose level.
These tests are affordable, widely available, and can identify the most common correctable causes of persistent tiredness within a single appointment. Many people discover that low ferritin or vitamin D, even within the conventional “normal” range, is a primary driver of their fatigue. Treating a low ferritin level alone, for example, has been shown in randomized controlled trials to reduce fatigue even in women who are not technically anemic.
Step 4: Address Your Stress Response Directly
Managing stress is not optional for people with fatigue that has a psychological or nervous system component. The following approaches have genuine clinical evidence behind them.
The Mindfulness-Based Stress Reduction (MBSR): An 8-week structured program that has been shown in multiple clinical trials to reduce fatigue severity, improve sleep quality, and lower inflammatory markers.
Diaphragmatic breathing: Slow, deep belly breathing activates the parasympathetic nervous system. Practicing 4-7-8 breathing or simple box breathing for 5 minutes twice daily has measurable effects on cortisol and heart rate variability within two weeks.
Progressive Muscle Relaxation (PMR): A technique of systematically tensing and releasing muscle groups that helps the body physically learn what “relaxed” feels like, useful for people whose stress response has become their default state.
Step 5: Move Your Body Strategically
Physical activity is one of the most consistently supported remedies for general fatigue in the research literature. A large meta-analysis published in the journal Psychological Medicine found that exercise interventions significantly reduced fatigue across multiple populations and health conditions.
The word “strategically” matters here. If you have ME/CFS or experience post-exertional malaise, aggressive exercise can worsen symptoms significantly. In that case, activity must be very carefully paced, ideally under medical supervision. For general chronic fatigue without PEM, aim for 20 to 30 minutes of moderate-intensity movement most days: brisk walking, swimming, cycling, or gentle yoga. Morning activity is especially beneficial because it helps reinforce your circadian rhythm and boosts daytime alertness without interfering with sleep.
The Food and Energy Connection That Most People Completely Miss
Food is not just comfort or pleasure. It is the literal fuel your mitochondria use to produce adenosine triphosphate (ATP), the molecule that powers every single cell in your body. When your diet is out of alignment with your body’s needs, energy production suffers at the cellular level, and no amount of sleep will compensate for that.
The Blood Sugar Roller Coaster
A diet heavy in refined carbohydrates, added sugar, and ultra-processed foods causes rapid spikes in blood glucose followed by sharp crashes. Those crashes trigger a stress hormone response (cortisol and adrenaline release) to stabilize blood sugar. This is uncomfortable, it disrupts sleep architecture, and it is responsible for the familiar mid-afternoon energy crash that millions of people experience as an unavoidable part of life. It is not unavoidable. It is dietary.
Shifting toward a diet built around whole foods, with protein, healthy fat, and complex carbohydrates at each meal, creates far more stable blood sugar throughout the day. This alone can produce a noticeable improvement in sustained energy within 1 to 2 weeks for many people.
Key Nutrients That Directly Impact Energy Production
Magnesium: Involved in over 300 enzymatic reactions in the body, including ATP synthesis. Many Americans do not meet the recommended daily intake. Rich dietary sources include pumpkin seeds, dark leafy greens, black beans, dark chocolate, and almonds.
CoQ10 (Coenzyme Q10): A compound produced naturally in the body that plays a central role in the mitochondrial electron transport chain (energy production). CoQ10 levels decline with age and may be depleted by statin medications commonly used for cholesterol management. It is available as a supplement, typically in doses of 100 to 200 mg daily.
B vitamin complex: The B vitamins (B1, B2, B3, B5, B6, B9, and B12) are all involved in converting food into usable energy. If you follow a predominantly plant-based diet, B12 supplementation is especially critical since it is found almost exclusively in animal products.
Omega-3 fatty acids (EPA and DHA): Found in fatty fish, sardines, and algae-based supplements, omega-3s reduce systemic inflammation, which is increasingly linked to both fatigue and poor sleep quality in the research literature.
UK / Canada / Australia note: In the UK, Public Health England recommends 10 micrograms (400 IU) of vitamin D daily for adults in autumn and winter months. Health Canada recommends 600 IU for adults. In Australia, recommendations vary by skin type and geographic UV exposure. Speak to your GP or pharmacist for a dose appropriate to your circumstances.
When to See a Doctor About Chronic Fatigue and Constant Tiredness
Self-guided lifestyle improvements are a smart starting point. But there are clear signs that what you are experiencing requires professional medical evaluation. Fatigue that significantly affects your ability to function is not something to simply push through and hope improves.
Seek medical attention if you experience any of the following:
Fatigue that has persisted for 6 weeks or more with no clear explanation
Fatigue severe enough to prevent you from completing normal daily activities
A clear pattern of feeling significantly worse after physical or mental activity (post-exertional malaise)
Fatigue accompanied by unintentional weight loss, night sweats, or persistent low-grade fever
Chest discomfort, palpitations, or shortness of breath appearing alongside fatigue
Depressive symptoms or any thoughts of harming yourself (in which case, please reach out to a crisis line or emergency services immediately)
When you go to that appointment, come prepared. Bring a log of your symptoms, their duration, your sleep patterns, and any relevant lifestyle factors. Ask your doctor to run the foundational fatigue blood panel: CBC, ferritin, vitamin B12, 25-hydroxyvitamin D, TSH with free T4, and fasting blood glucose. Being specific about what you want tested increases the likelihood of finding an actionable answer.
Real-World Example
How Marcus Found His Way Out of Three Years of Exhaustion
Marcus was 42, a project manager based in Denver, and had been waking up tired every single morning for nearly three years. He was getting between 7.5 and 8.5 hours of sleep a night by all accounts. He was not staying up late, he was not drinking heavily, and he exercised a few times a week. On paper, he was doing everything right. In practice, he was dragging himself through every workday and collapsing on the couch by 7 PM.
After two separate doctors told him his bloodwork was “fine” and suggested he try reducing his stress levels, Marcus pushed for a more detailed panel. The results were revealing. His ferritin was 11 ng/mL (low-normal by conventional standards, but many practitioners consider anything below 50 ng/mL suboptimal for men experiencing fatigue). His 25-hydroxyvitamin D was 19 ng/mL. His TSH was within normal limits but on the higher end, and a follow-up free T4 test suggested his thyroid was underperforming.
His treatment plan included daily ferrous sulfate supplementation (325 mg taken with vitamin C to boost absorption), 3,000 IU of vitamin D daily, and a thyroid recheck in 12 weeks. His doctor also referred him for a home sleep study after Marcus mentioned that his wife had commented on occasional snoring. The sleep study identified mild to moderate sleep apnea, and he was fitted with a CPAP device.
Within 3 months, Marcus reported that his energy levels were “genuinely better than they had been in years.” His ferritin had risen to 48 ng/mL, his vitamin D to 44 ng/mL, and his morning grogginess had dropped significantly after 6 weeks on the CPAP. He still had days that were harder than others, but the weight of daily exhaustion had lifted in a way that felt almost unfamiliar at first. “I had forgotten what it felt like to actually wake up and feel okay,” he said.
This is a composite example based on commonly observed clinical patterns. It is provided for illustrative purposes only. Individual results will vary. Always work with your own healthcare provider for personalized diagnosis and treatment.
Frequently Asked Questions About Chronic Fatigue
Can you have ME/CFS without realizing it?
Yes, and it is more common than most people realize. ME/CFS is significantly underdiagnosed, partly because its symptoms overlap with many other conditions, and partly because there is still no definitive blood test or imaging finding that confirms the diagnosis. The CDC estimates that up to 91% of Americans with ME/CFS have not received a formal diagnosis.
The most distinguishing feature of ME/CFS compared to other fatigue conditions is post-exertional malaise (PEM), a significant worsening of all symptoms following even modest physical or mental activity that tends to last 24 hours or longer. If this pattern sounds familiar, bring it up explicitly with your doctor and ask about the Institute of Medicine’s 2015 diagnostic criteria, which is the most current clinical standard used in the US, UK, Canada, and Australia.
Is waking up tired after 8 hours always a sign of a medical problem?
Not always. Occasionally waking up unrefreshed is normal, especially during or after periods of high stress, illness, heavy travel, or major life changes. The key word is “occasionally.” When it happens most mornings, week after week, that is when your body is flagging something worth investigating.
Start with lifestyle factors first. Consistent sleep and wake times, reducing caffeine after noon, getting morning sunlight, and managing stress are genuinely effective for many people and can show results within 2 to 4 weeks. If improving those factors does not produce noticeable improvement, or if your fatigue is severe enough to affect your daily functioning, schedule an appointment with your doctor and ask for a thorough fatigue workup. Persistent unrefreshing sleep is not something to simply accept as your new normal.
What is the fastest natural approach to improving fatigue?
Two changes tend to produce results fastest for most people. The first is consistent morning sunlight exposure, ideally 10 to 20 minutes outdoors within an hour of waking. This resets the circadian clock, improves melatonin timing at night, and lifts morning grogginess. Many people notice a difference within 5 to 7 days.
The second is improving hydration. Even mild dehydration, as little as 1 to 2% of body weight in fluid deficit, has been shown in controlled research to impair mood, concentration, and perceived energy. Most adults function best with approximately 8 to 10 cups (2 to 2.5 liters) of water daily, adjusted upward for hot weather, exercise, and body size. These are not cures for underlying medical conditions, but they address genuine lifestyle contributors that are extremely common and genuinely fixable.
Conclusion: Chronic Fatigue Is Explainable, and In Most Cases, It Is Fixable
If you have been waking up exhausted after a full night of sleep, this article has one central message for you: this is not normal, and it is not something you simply have to accept as the way things are for you now.
Chronic fatigue after sleeping is a signal. It is telling you that something in the picture is out of alignment, whether that is your sleep quality, your hormone levels, your nutrition, your body’s stress response, or an underlying condition that has not yet been identified. All of those have real causes, and most of them have real solutions.
The most important takeaways from this article are these. Sleep duration and sleep quality are not the same thing. Nutritional deficiencies, sleep disorders, thyroid imbalances, and chronic nervous system hyperarousal are among the most common and most treatable drivers of persistent tiredness. Lifestyle changes, when applied consistently and correctly, can make a meaningful difference. And when they are not enough on their own, a targeted blood panel and honest conversation with a doctor are the right next step.
Your energy is not a luxury item. It is the foundation of everything else you want to do and feel in your life. With the right information and the right support, most people can get a significant portion of it back. Start with one step from this article today. Consistency over perfection, always.
Medical Disclaimer: This article is written for educational and informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always speak with a qualified healthcare provider before making any changes to your health routine. If you are experiencing severe or worsening fatigue, please seek medical attention.